Billing Code Guide
Why Am I Being Balance-Billed for an In-Network Dental Procedure?
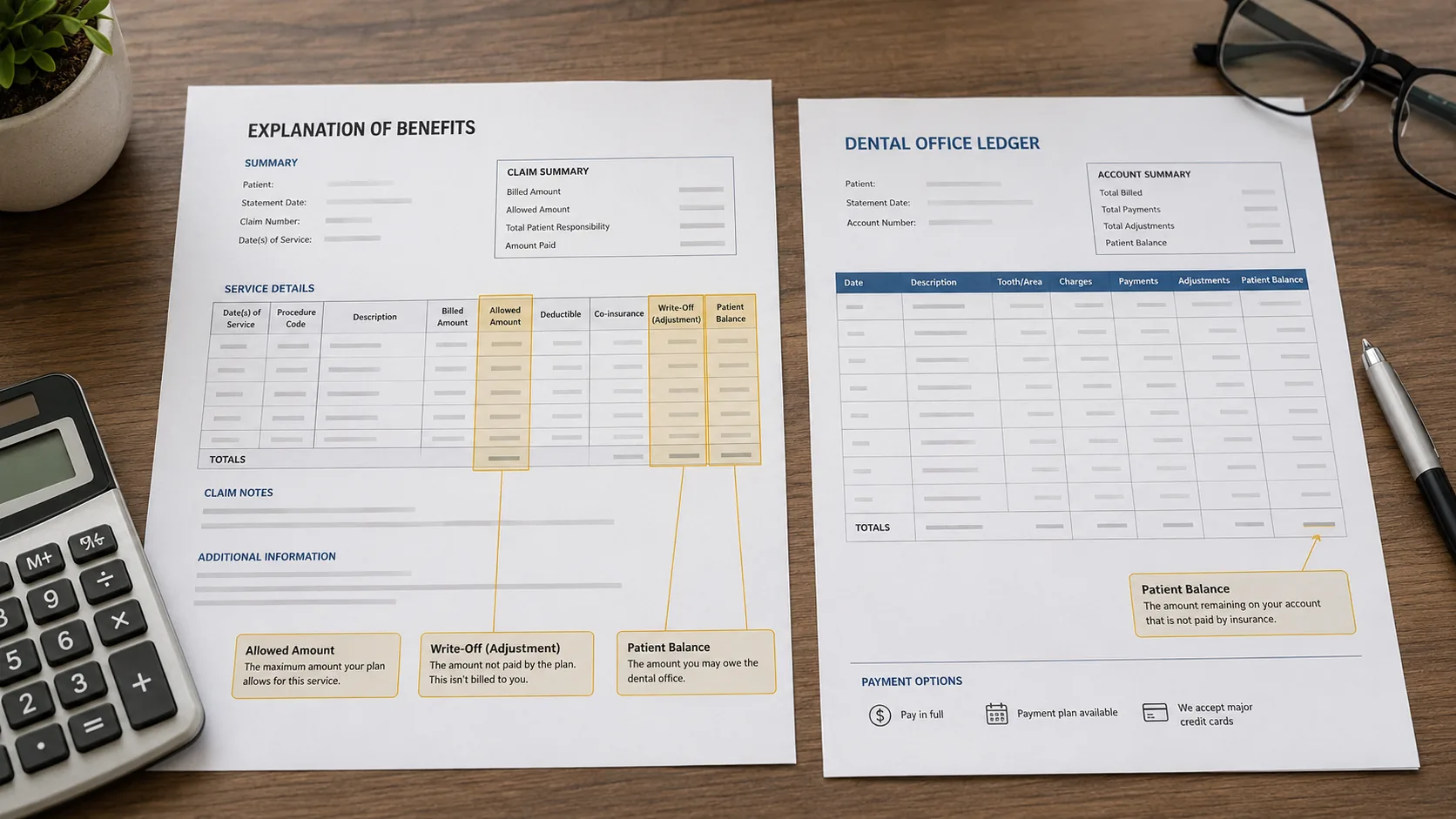
In-network dental offices generally must reconcile patient balances against allowed amounts, write-offs, deductibles, copays, and coinsurance shown on the EOB.
Executive Summary
Quick Summary- An in-network dental balance bill is worth disputing when the practice ledger asks you to pay more than the EOB says you owe after allowed amount, write-off, deductible, copay, and coinsurance.
- The central document is the EOB. It should reconcile to the practice ledger line by line.
- Ask the office to identify the contractual basis for any balance above patient responsibility.
- GetTrueCharge can compare the ledger and EOB to draft a balance-billing dispute.
Check your exact bill
Upload your dental ledger. We show a free preview of the strongest code, balance, or unbundling issue before checkout.
Direct answer
Your EOB Is the Control Document
If the dentist was in-network, your balance should generally track the EOB's patient responsibility fields. If the practice tries to collect the difference between its full fee and the plan's allowed amount, the dispute should demand a ledger-to-EOB reconciliation.
| Field | Meaning | Dispute use |
|---|---|---|
| Allowed amount | Contracted rate for the service | Compare to ledger charge |
| Adjustment or write-off | Amount provider may need to remove | Should not reappear as patient balance |
| Patient responsibility | Deductible, copay, or coinsurance | Maximum amount to reconcile |
Evidence
Ask for a Ledger-to-EOB Reconciliation
- Full EOB for the procedure date.
- Practice ledger showing charges, payments, adjustments, and current balance.
- Network status confirmation from insurer.
- Written explanation for any balance above EOB patient responsibility.
Have the EOB?
Audit the balance bill
Action
Make the Office Put the Basis in Writing
Request
Please reconcile this ledger balance to the EOB and identify the contractual basis for billing any amount above the EOB patient responsibility.
Frequently Asked Questions
Can an in-network dentist ever bill me after insurance?
Yes, for valid deductibles, copays, coinsurance, or non-covered services. The concern is billing more than the EOB and contract allow.
What if the office says insurance is wrong?
Ask the office and insurer to reconcile the claim in writing. Keep both responses with your ledger and EOB.
Should I pay while the dispute is pending?
That depends on timing and collection risk. At minimum, put the dispute in writing and keep proof of your reconciliation request.
Sources Cited
D4341 D4342 Coding for Periodontal Scaling and Root Planing
American Dental AssociationADA practice guidance on scaling and root planing code use, documentation, and payer review.
Guide to Extractions
American Dental AssociationADA extraction coding guide used for understanding extraction-related procedure reporting.
Dental Radiographic Examinations Policy
AetnaDental radiographic policy context for full-mouth, panoramic, bitewing, and diagnostic image review.
Balance Billing Best Practices
Delta DentalProvider-facing guidance on avoiding improper patient billing and balance-billing disputes.
Provider Manual: Hold Harmless and Balance Billing
Health Net Provider LibraryHealth plan manual example explaining hold-harmless principles and provider limits on billing members.
Disclaimer
This article is educational information, not legal, financial, dental, medical, or insurance advice. Dental billing rules vary by payer, provider, plan, state, and facts. GetTrueCharge provides document review and dispute drafting support, but does not guarantee a refund or invoice adjustment.
Related Audits
Dentist Billed Separately for a Core Buildup and a Crown? Why You're Being Double-Billed
A core buildup can be separate only when the tooth lacks enough structure to support a crown. Ask for radiographs, clinical notes, and the EOB before paying the extra balance.
Read guide
Charged for a Full Mouth X-Ray and 4 Bitewings on the Same Day? Spot Diagnostic Double-Dipping
A full-mouth series often includes bitewing views. If both appear on the same date, ask for image files, clinical necessity, and EOB bundling logic.
Read guide
Dentist Billed My Insurance for Scaling and Root Planing but Only Did a Basic Cleaning
Scaling and root planing should be supported by periodontal charting, bone-loss evidence, and clinical notes. Ask for the perio record before paying the higher balance.
Read guide
Charged $150 for Local Anesthesia That Should Have Been Included in the Extraction Fee
Local anesthesia is often included in extraction procedures. If it appears as a separate patient charge, ask for the CDT rationale, EOB handling, and anesthesia record.
Read guide