Billing Code Guide
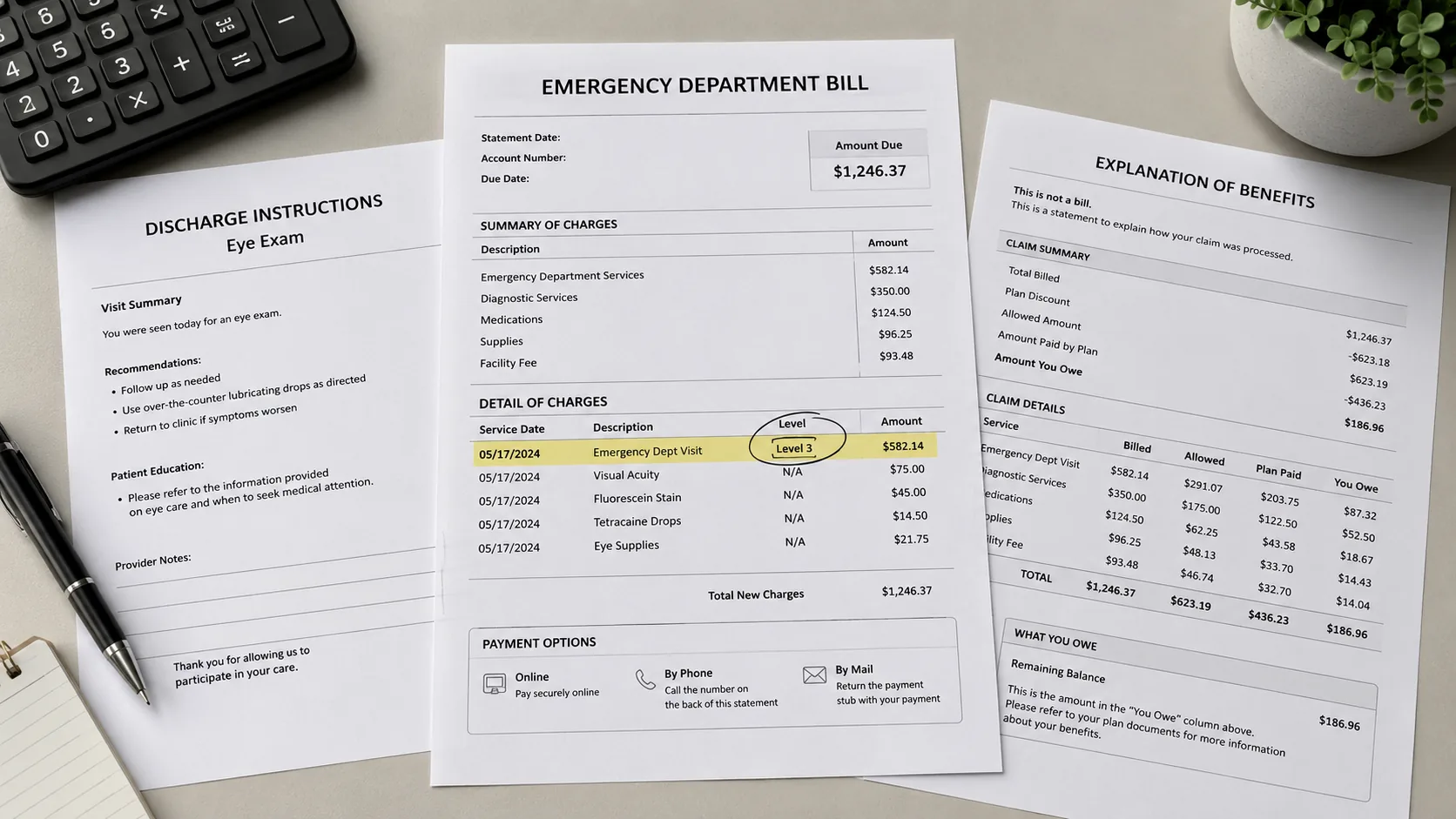
Billed $1,150 for a Level 3 ER Visit After Just an Eye Exam: How to Fight Back
A Level 3 ER visit should reflect documented evaluation and resource use. If the visit was a simple eye exam, request the chart and facility-level rationale.
Executive Summary
Quick Summary- A $1,150 Level 3 ER charge after a simple eye exam is worth disputing when the chart does not show moderate complexity, testing, treatment, or resource use supporting that level.
- Ask for the itemized bill, physician note, nursing note, orders, treatment record, discharge summary, and facility-level rationale.
- The dispute should say the code may be unsupported by the record, not merely that the price is high.
- GetTrueCharge can scan the bill and draft a Level 3 review request tied to the actual line item.
Check your exact bill
Upload your bill or EOB. We show a free preview of the strongest billing issue before you decide to unlock the dispute packet.
Direct answer
A Minor Visit Can Still Be Overleveled
Level 3 ER billing often sits in the gray zone. It may be appropriate for moderate evaluation, but if the record shows only a quick eye exam, no meaningful testing, no medication beyond basic treatment, and straightforward discharge, the patient should ask why Level 3 was selected.
| Record | Supports level when | Red flag |
|---|---|---|
| Provider note | Moderate decision making is documented | Brief uncomplicated eye exam |
| Orders | Testing or treatment beyond simple exam | No labs, imaging, or procedure |
| Discharge record | Follow-up and risk are documented | Routine instructions only |
Evidence
Request the Facility-Level Rationale
- Itemized bill showing the Level 3 line and amount.
- Complete provider and nursing notes for the visit.
- Orders, tests, medications, or procedures billed for the encounter.
- Written coding rationale or facility-level review.
Have the ER statement?
Audit the Level 3 charge
Action
Ask for Releveling if the Chart Is Thin
Request
Please provide the documentation and facility-level rationale supporting the Level 3 emergency department charge. If the record supports a lower visit level, please recode and reprocess the patient balance.
Frequently Asked Questions
Is Level 3 always wrong for an eye complaint?
No. Some eye complaints can involve risk, testing, medication, or specialist concern. The dispute depends on what the chart shows.
Can a hospital lower an ER visit level?
Hospitals can review coding and issue corrected claims or statements when documentation does not support the original level.
What is the strongest evidence?
The itemized bill plus the complete ER record. Together they show the billed level and the care actually documented.
Sources Cited
No Surprises Act consumer protections
Centers for Medicare & Medicaid ServicesFederal guidance on surprise billing protections, emergency services, and consumer dispute paths.
Hospital Price Transparency
Centers for Medicare & Medicaid ServicesCMS requirements for hospital standard charges and consumer-friendly pricing information.
Medicare Claims Processing Manual
Centers for Medicare & Medicaid ServicesPrimary CMS manual source for claims-processing context and billing documentation expectations.
Coding intensity and evaluation management oversight
U.S. Department of Health and Human Services Office of Inspector GeneralOIG work-plan context for evaluation and management billing review and upcoding oversight.
Disclaimer
This article is educational information, not legal, medical, financial, or coding advice. Billing rules vary by payer, provider, state, and facts. GetTrueCharge provides document review and dispute drafting support, but does not guarantee a billing adjustment.
Related Audits
How to Dispute CPT 99285 on an Emergency Room Bill
Learn when CPT 99285 may be worth questioning, what evidence to request, and how to route your bill into GetTrueCharge for a charge-specific audit.
Read guide
How the No Surprises Act Applies to Emergency Room Bills
A practical guide to No Surprises Act signals on ER bills, including out-of-network physicians, facility-based charges, and documentation requests.
Read guide
How to Request an Itemized Hospital Bill Before Paying
Use this checklist to request CPT codes, facility charges, supplies, administrative fees, taxes, and EOB reconciliation before paying a hospital bill.
Read guide
Charged for a Level 5 ER Visit but Only Saw a Nurse for 8 Minutes? How to Spot Upcoding
A Level 5 ER charge should be supported by high-complexity emergency documentation. If the record shows brief triage care, request the chart, facility-level matrix, and coding rationale.
Read guide
Why Your Hospital Bill Has Two Separate Charges for the Same Doctor Visit
A provider fee and facility fee can appear for one visit. Dispute the facility fee when the site, notice, EOB, or provider-based status does not support the extra charge.
Read guide
My Hospital Bill Has a $9,000 Observation Charge and I Was Never Admitted
Observation status can create large outpatient charges. Ask for the observation order, MOON notice when applicable, hourly codes, and admission-review rationale.
Read guide
Hospital Charged Me for Tests I Never Got: CT Scan, Labs, EKG, and How to Prove It
A test charge should match an order, result, report, or chart entry. If the bill lists tests you never received, request the medical record and itemized code support.
Read guide